Abnormal liver profile and autoimmune liver disease
Overlap Syndromes
As the name suggests, overlap syndromes are clinical conditions in which patients have features of more than one autoimmune liver diseases, in this patient’s case, PBC and AIH. These conditions are rare and AIH-PBC is the most common, occurring in 1-3% of PBC patients and up to 7% of AIH patients. An overlap syndrome should be suspected in patients with a predominant disease such as AIH, PBC, PSC, but with atypical biochemical, serological, or histological features. These patients may respond differently to conventional treatments directed solely at the predominant condition.
Diagnostic Criteria
PBC should be investigated in patients with chronic cholestasis manifesting as an elevated alkaline phosphatase (ALP). Diagnosis requires two of the following: (1) ALP elevation, (2) positive anti-mitochondrial antibody (AMA) or positive sp100 or gp210 antibodies if AMA is negative (noted in 5-10% of patients), and (3) histology showing nonsuppurative destructive cholangitis with interlobular and septal bile duct destruction, focal lesions with inflammatory changes and necrosis (the “florid duct lesion”), and inflammatory infiltrate near cholangiocytes. In patients without cirrhosis, the degree of ALP elevation correlates to the severity of bile duct damage. Importantly, a liver biopsy is not required to diagnose PBC, but is recommended to exclude other concomitant entities when atypical findings are present.
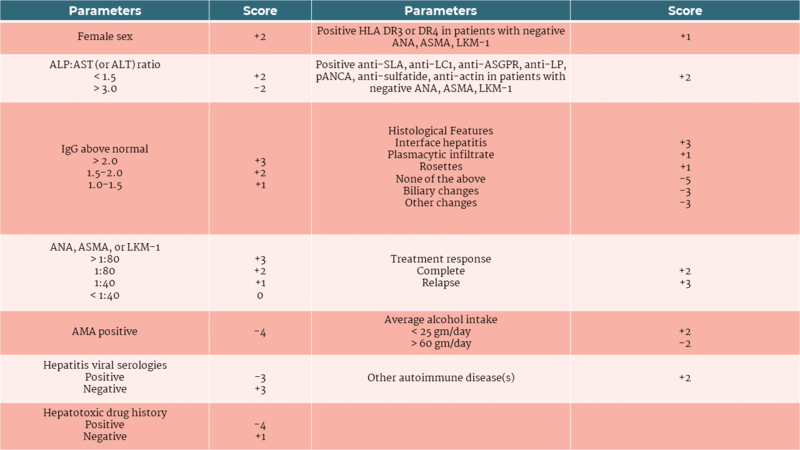
Patients with suspected AIH should have viral hepatitis, drug-induced liver injury, hereditary, and metabolic disorders ruled out as these conditions may resemble AIH. Diagnosis is based on histology showing interface hepatitis with plasma cell infiltration and lobular hepatitis possibly with centrilobular necrosis and hepatocyte rosettes in addition to (1) elevated AST/ALT levels, (2) elevated IgG level and/or the presence of autoantibodies such as ANA, ASMA, and anti-LKM1, and (3) the exclusion of disorders listed above. The presence of two autoantibodies (ANA and ASMA) significantly increases the diagnostic accuracy for AIH. Anti-LKM1 is often found in patients who are ANA and ASMA negative and should be obtained after first testing for ANA and ASMA if suspicion for AIH remains elevated. The revised scoring system for AIH was developed by the International Autoimmune Hepatitis Group and is based on several clinical and laboratory variables as shown in Table 1. A score above 15 indicates a definite diagnosis of AIH and a score of 10-15 indicates a probable diagnosis. All patients with AIH should be screened for celiac and thyroid diseases at time of diagnosis.
Table 1- Revised AIH scoring system
Abbreviations: ALP, alkaline phosphatase; AST, aspartate transaminase; ALT, alanine transaminase; ANA, antinuclear antibody; ASMA, anti-smooth muscle antibody; anti-LKM1, anti-liver kidney microsomal type 1 antibody; AMA, antimitochondrial antibody; IgG, immunoglobulin G; anti-SLA, anti-soluble liver antigen antibody; anti-LC1, anti-liver cytosol antibody type 1 antibody; anti-ASGPR, anti- asialoglycoprotein receptorantibody; anti-LP, anti-liver pancreas antibody; pANCA, perinuclear anti-neutrophil cytoplasmic antibody
AIH-PBC overlap is diagnosed by applying the Paris criteria to patients with PBC. These patients with PBC must have two of the following: (1) ALP ≥ 2*ULN or GGT ≥ 5*ULN, (2) positive AMA, and (3) florid duct lesion on biopsy. One caveat is that the Paris criteria does not capture patients who have less severe cholestasis (those with a mildly elevated ALP), and therefore, the diagnosis of overlap should not be entirely excluded. In order to assess for AIH in the setting of PBC, liver biopsy must show moderate or severe interface hepatitis with either (1) ALT ≥ 5*ULN or (2) IgG ≥ 2*ULN and/or positive ASMA in order to diagnose PBC-AIH overlap. The Paris criteria are 92% sensitive and 97% specific for PBC-AIH overlap syndrome. Table 2 summarizes diagnostic criteria for the above autoimmune liver conditions. A new AIH-PBC overlap scoring system combines clinical, laboratory, and histology results (similar to the revised AIH score) and was shown to have a sensitivity of 98.5% and specificity of 92.8% in a single-center study. A diagnostic algorithm is presented in Figure 1.
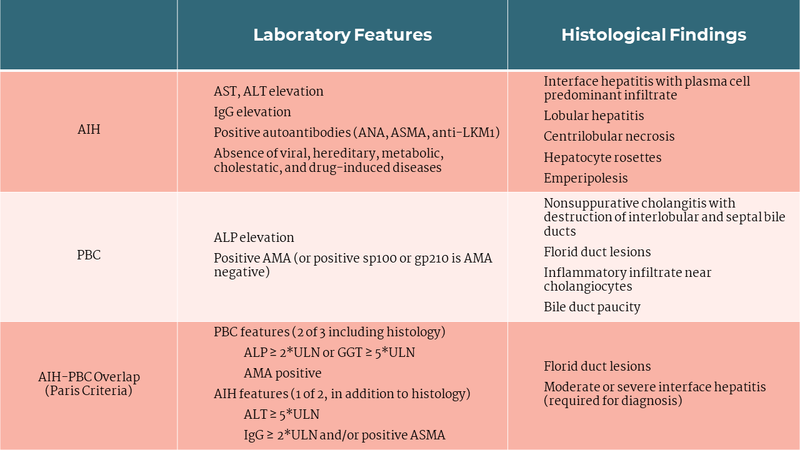
Table 2: Features of several autoimmune liver diseases
Abbreviations: AIH, autoimmune hepatitis; PBC, primary biliary cholangitis; ALP, alkaline phosphatase; AST, aspartate transaminase; ALT, alanine transaminase; ANA, antinuclear antibody; ASMA, anti-smooth muscle antibody; anti-LKM1, anti-liver kidney microsomal type 1 antibody; AMA, antimitochondrial antibody
Figure 1: Diagnostic algorithm in evaluation of overlap syndromes
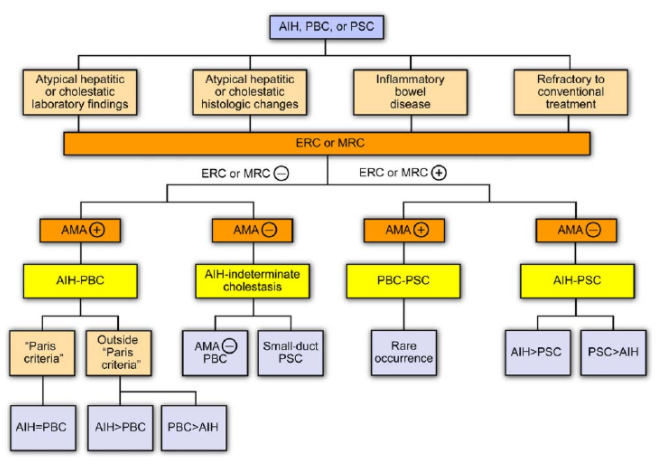
Adapted from: Czaja AJ. Overlap syndromes. Clinical Liver Disease. 2014.
Abbreviations: AIH, autoimmune hepatitis; PBC, primary biliary cholangitis; PSC, primary sclerosing cholangitis; ERC, endoscopic retrograde cholangiography; MRC, magnetic resonance cholangiography; AMA, antimitochondrial antibody
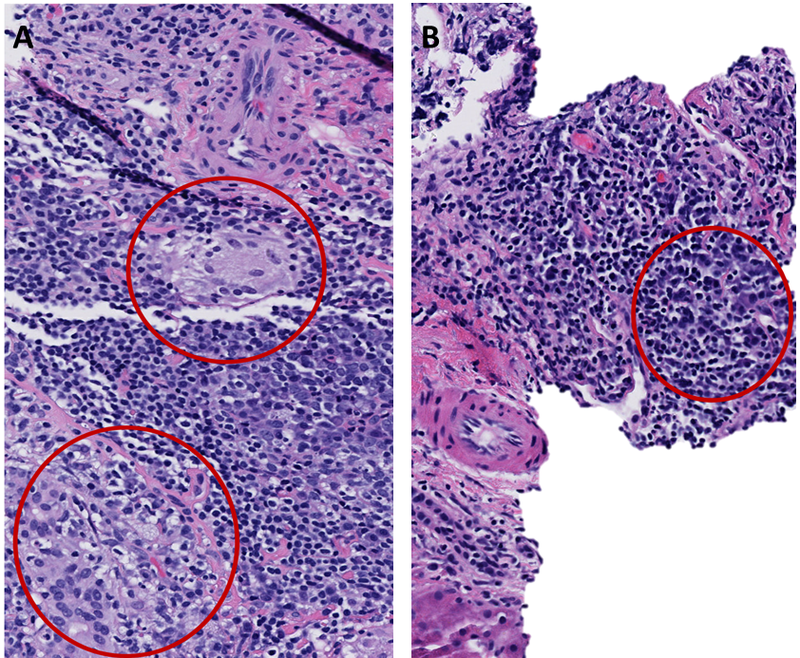
Figure 2 -Pathology slides demonstrating bile duct destructive non-caseating portal granuloma (A, upper circle) and bile ductular proliferation (A lower circle) and plasma cell rich portal infiltrate (B).
Treatment
PBC patients often present with fatigue and pruritus. The mainstay of treatment is indefinite ursodeoxycholic acid (UDCA), dosed at 13-15mg/kg/day which has been shown to improve lab parameters, delay histologic disease progression, and transplant-free survival. ALP and bilirubin correlate to treatment response and labs generally improve within months. UDCA does not improve symptoms of PBC such as pruritus and fatigue. Obeticholic acid (OCA) is a farsenoid X receptor agonist that reduces bile acid synthesis. OCA can be used in combination with UDCA in patients with compensated PBC who have poor response to UDCA, as defined by persistently elevated ALP after one year of treatment, or as monotherapy in patients with UDCA intolerance. In a phase 3 study, OCA was shown to reduce ALP, however it also worsened pruritus in a dose-dependent manner. The goal of treatment is to attain normal ALP and bilirubin levels as these have been associated with a lower risk of death and need for liver transplantation. Pruritus can be managed with anion-exchange resins such as cholestyramine (to be administered one hour after medications) and colestipol, or with naltrexone or rifampicin.
AIH patients often present with fatigue and malaise and up to one-third of adults have cirrhosis upon presentation. The goal of treatment is to prevent disease progression and attain biochemical remission by normalizing AST, ALT, and IgG levels. Induction is with prednisone monotherapy or with combination prednisone and azathioprine therapy. Thiopurine methyltransferase activity should be assessed prior to starting azathioprine. Labs should be obtained frequently to assess for treatment response and to monitor for the development of cytopenias that would necessitate azathioprine dose reduction or withdrawal. Azathioprine should be avoided in decompensated cirrhosis due to the risk of cytopenias. Budesonide is an alternative to prednisone in combination therapy with azathioprine and was shown to achieve biochemical remission sooner and with fewer steroid-related adverse effects (particularly bone mineral disease). Budesonide should be avoided in patients with cirrhosis as portosystemic shunting may reduce drug effect and cases of thrombotic events have been reported. Importantly, budesonide and azathioprine should be avoided in acute severe AIH or acute liver failure. As labs show improvement, steroids should be tapered. The rapidity of response to treatment is the single most important predictor of outcomes and transaminases should improve within two weeks of initiation. Remission within six months is associated with lower disease progression to cirrhosis and need for liver transplantation. A recent multicenter study concluded that lower aminotransferases during AIH treatment were associated with improved long-term survival and reemphasized the necessity of biochemical remission.
AIH-PBC overlap is treated with UDCA in addition to prednisone monotherapy or prednisone and azathioprine therapy. Combination therapy has been shown to improve biochemical tests, stabilize fibrosis, and preserve 5-year transplant free survival. Additionally, combination therapy is superior to prednisone alone and UDCA alone as determined by this meta-analysis. The presence of severe interface hepatitis was found to be a predictor of failure to achieve remission on UDCA monotherapy, supporting the use of immunosuppression in this patient population. A study comparing 26 AIH-PBC overlap patients to 135 PBC patients discovered more significant portal hypertension, increased mortality, and higher need for liver transplantation in the overlap group. More studies with larger study populations are needed.